Clinical diagnosis is a crucial component of healthcare services, constituting an estimated 3-5% of overall healthcare spend. It is estimated that about 70% of clinical decisions are taken based on lab results. Development of sophisticated and specialised tests for early disease detection and disease management, and the increasing demand for lab automation are the key drivers of clinical diagnostics market.
According to a first-of-its-kind study by The World Bank Group and the Institute for Health Metrics and Evaluation (IHME) at the University of Washington, that detailed and drew comparisons on total health spending across income levels and geographies through the year 2040 for 184 low, middle, and high-income countries, more resources are expected to be spent on health in the future – with a projected $18.28 trillion, or 9% of global GDP, allocated to health spending by 2040.
The report also predicts a widening health spending divide between the world’s poorest and wealthiest countries. It indicates that many countries which are grappling with the largest and most complex disease burdens will spend the least on health.
The dual challenge for healthcare policy and practice is to:
- Reduce misuse and wasteful clinical diagnosis in the mature economies
- Enable greater access to quality and affordable diagnostic tools in the emerging economies

The waste and inequities in global healthcare spend is further compounded by the additional factor of a fast-ageing population – and nowhere is this trend more pronounced than in Asia. According to the World Economic Forum, the aged population in the region will increase from 414 million in 2010 to almost 1.3 billion by 2050, representing two-thirds of the world’s older people.
Example of Disease Diagnosis at Scale and Impact
Diabetic retinopathy (DR), a major microvascular complication of diabetes, has a significant impact on the world’s health systems. Globally, the number of people with DR will grow from 126.6 million in 2010 to 191.0 million by 2030, and it is estimated that the number with vision-threatening diabetic retinopathy (VTDR) will increase from 37.3 million to 56.3 million, if prompt action is not taken.
A good example of healthcare innovation is IDx-DR, the first AI-based medical device approved by FDA to automatically detect diabetic retinopathy. Images of the patient’s retina are captured by a Topcon NW400 camera and uploaded to a cloud server, where the IDx-DR software resides. IDx-DR is the first device authorised for marketing that provides a screening decision without the need for a clinician to also interpret the image or results, which makes it usable by healthcare providers who may not normally be involved in eye care.
The FDA evaluated data from a clinical study of retinal images obtained from 900 patients with diabetes at 10 primary care sites. The study was designed to evaluate how often IDx-DR could accurately detect patients with more than mild diabetic retinopathy. In the study, IDx-DR was able to correctly identify the presence of more than mild diabetic retinopathy 87.4 % of the time and was able to correctly identify those patients who did not have more than mild diabetic retinopathy 89.5 % of the time.
AI based systems are set to revolutionise healthcare by providing high quality clinical diagnostics at a far greater scale than before, democratising access to those in need, and at a cost that makes it valuable for all the stakeholders.
Digital Health Ecosystem
The promise of AI is clearly not lost on the industry. Rock Health, the first venture fund dedicated to Digital Health, suggests that H1 2018 saw 193 Digital Health firms raise funding worth US$3.4 billion across America alone, putting funding on track to beat 2017 records.
What’s more, regulators around the world are slowly but surely easing requirements for novel and cutting edge technologies to enter the market – two recent examples include the FDA’s Digital Health Innovation Action Plan and Early Feasibility Study (EFS) programme in the US.
A recent study by Ecosystm shows that the applications of AI technologies in the MedTech space are far-reaching, with current focus areas including non-invasive diagnostics, remote health, clinical decision support and predicting patient risk. This would mean better flagging when serious illnesses and ailments are on the horizon, all the while minimising unnecessary consultations and reducing the workloads of already stretched healthcare professionals.
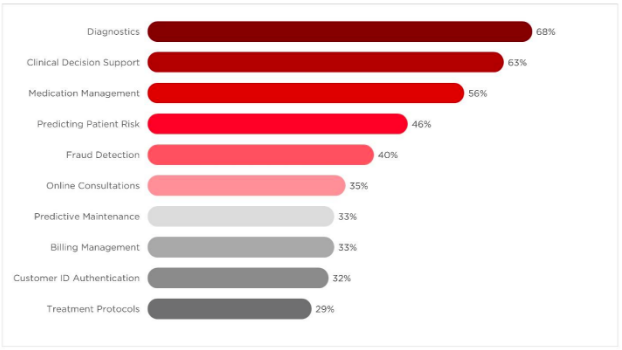
Source: Ecosystm, 2018. Top Business Solutions Addressed by AI in Healthcare Provider Organisations
What is Holding AI Back Then?
From a technological perspective, senior executives – CIOs and Line of Business leaders– cite integration with internal systems, access to data and cyber security as key challenges. To combat this, countries such as Singapore, Australia and New Zealand are looking at ways to aggregate and analyse digitised patient data in the hope of generating insights to improve clinical outcomes. More work needs to be done to understand specific concerns of all stakeholders, and resolve those conflicts in a respectful and pragmatic manner.

Source: Ecosystm, 2018. Top Challenges in AI Adoption in Healthcare Provider Organisations
That said, as pressures mount on the healthcare industry to achieve more with less, make no mistake that AI in healthcare is inevitable. We’re in a race against time – China, Hong Kong, Singapore, Japan, and India are just a few of the many countries across Asia that have cited shortages in healthcare manpower over the past year. As the elderly population increases, bringing with them a ream of age-related health issues, the situation is only going to get worse. So ready or not, it may well be the case that in a few short years, the healthcare industry will consider their AI-driven diagnostic tools as essential as their physical ones.
Closing themes
- AI is a great enabler to democratise disease diagnosis at a scale, cost and quality never been possible before
- While still an emerging field. trust is slowly developing. Some of the recent use cases are a step in the right direction
- Regulatory authorities are supporting the development by enabling and encouraging innovation
- Governments are removing roadblocks and barriers, in some cases, opening population health data sets to teach AI systems
- Patients are benefiting from improved access and quality
- Early adopters among providers are embracing new technology, but with caution – impact on payers is still to be seen




